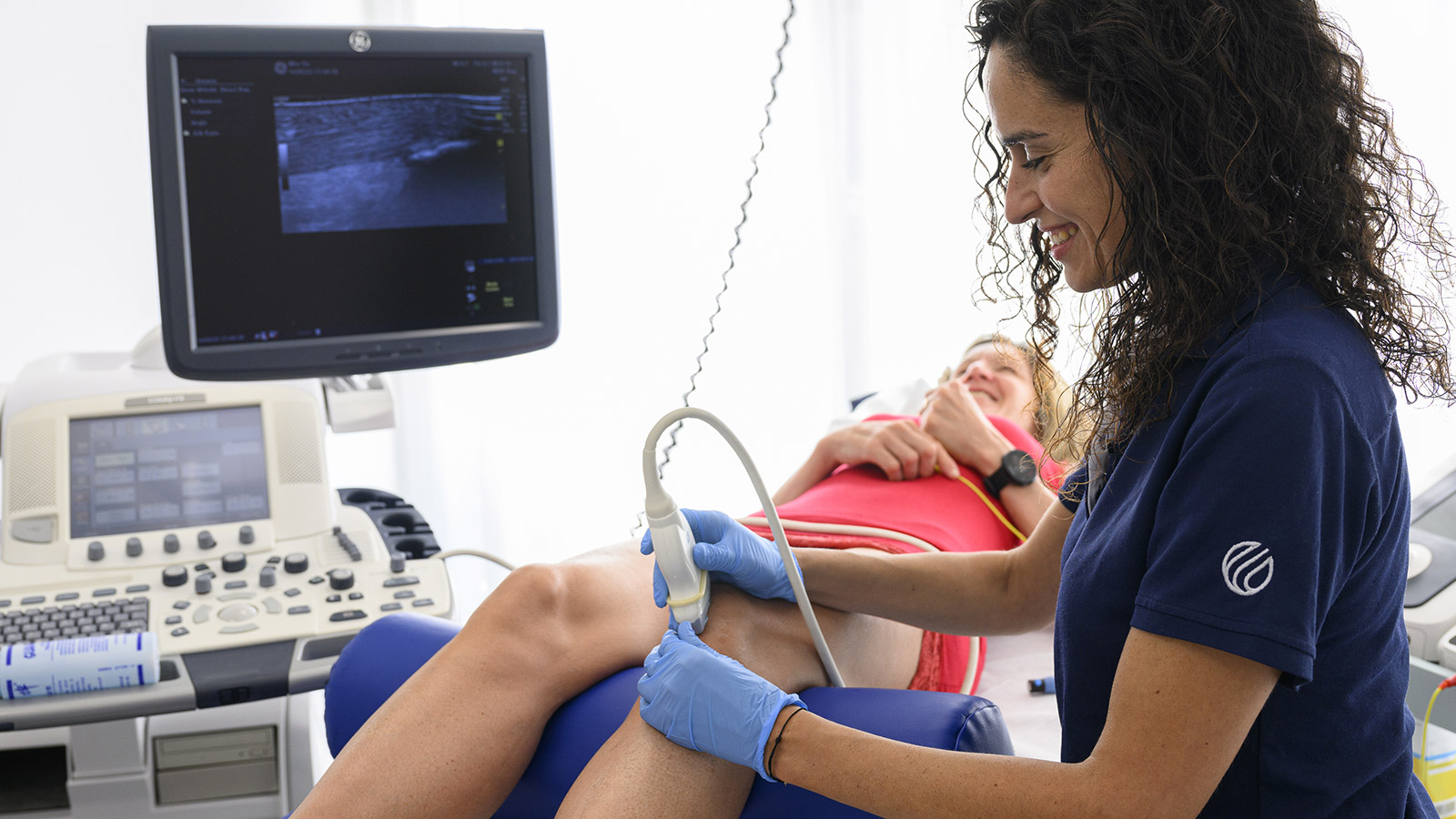
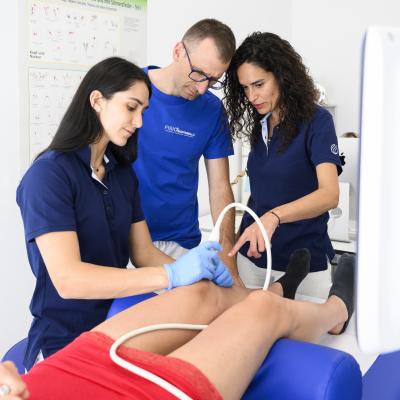
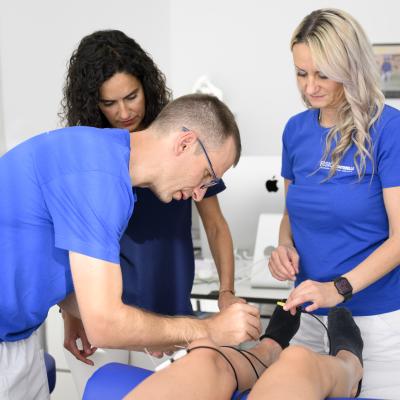
Percutaneous musculoskeletal electrolysis (EPM) is a technique that belongs to the invasive physiotherapy. It is very precise because of the ultrasound guidance and involves the targeted application of a galvanic current through an acupuncture needle at the site to be treated, which evokes an acute, controlled, local inflammatory process, which in turn allows phagocytosis of the damaged tissue and repair of the affected soft tissue. The EPM technique, compared with the EPTE technique (low-voltage current), uses high amperage currents, leading to excellent results in terms of modifying and improving the quality of the damaged tissue. Compared with the EPI® brand, the EPM methodology has generated treatment protocols supported by scientific basis.
It is very effective and greatly increases the therapy effectiveness, especially in cases of chronic pain. Usually, the results of EPM are seen already after one or two treatments; the technique is applied once a week and the treatment lasts 45 to 60 minutes.
Other physiotherapeutic forms are used as a complement to this technique, such as muscle strengthening and stimulation of neuromuscular control through active exercises and other conventional physiotherapeutic treatments (myofascial treatments, diathermy...).
This technique is practiced by a therapist specialized in musculoskeletal invasive physiotherapy (MIP), who, in order to practice it, must first take a course in musculoskeletal ultrasound (minimum 30 hours) and then the EPM course (60 hours). This training is also included in a university master's course that takes place in Spain, at the University San Pablo – Madrid (60 ECTS). During the training all the techniques of invasive physiotherapy are learned, which aim to treat soft tissues such as tendons, muscles, capsules, bursae, nerves and ligaments.
The technique is relatively new: it has been applied in Spain since 2008. The inventor of the technique is Jose Manuel Sánchez-Ibáñez, who registered the trademark EPI®. Later, Francisco Minaya-Munõz and Fermín Valera-Garrido developed the EPM application methodology, which today is the most scientifically validated approach. Francisco Minaya-Munõz and Fermín Valera-Garrido formed the MVClinic, who, in collaboration with the University San Pablo – Madrid, developed protocols for the treatment of each individual structure based on clinical and laboratory studies. In ten years, they trained many Spanish physiotherapists and thus greatly increased the chances of recovery for patients, especially where other physiotherapy techniques had previously failed.
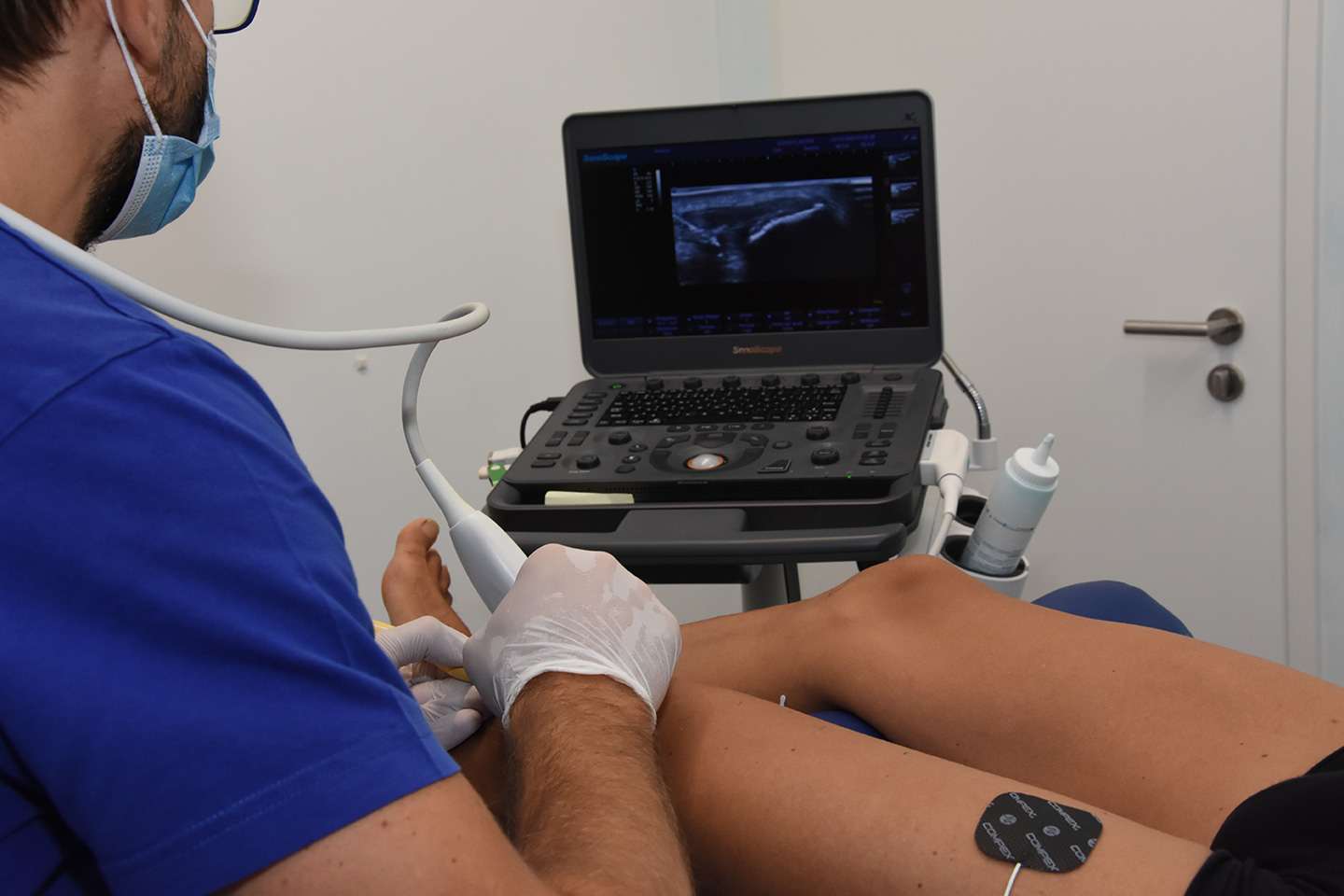
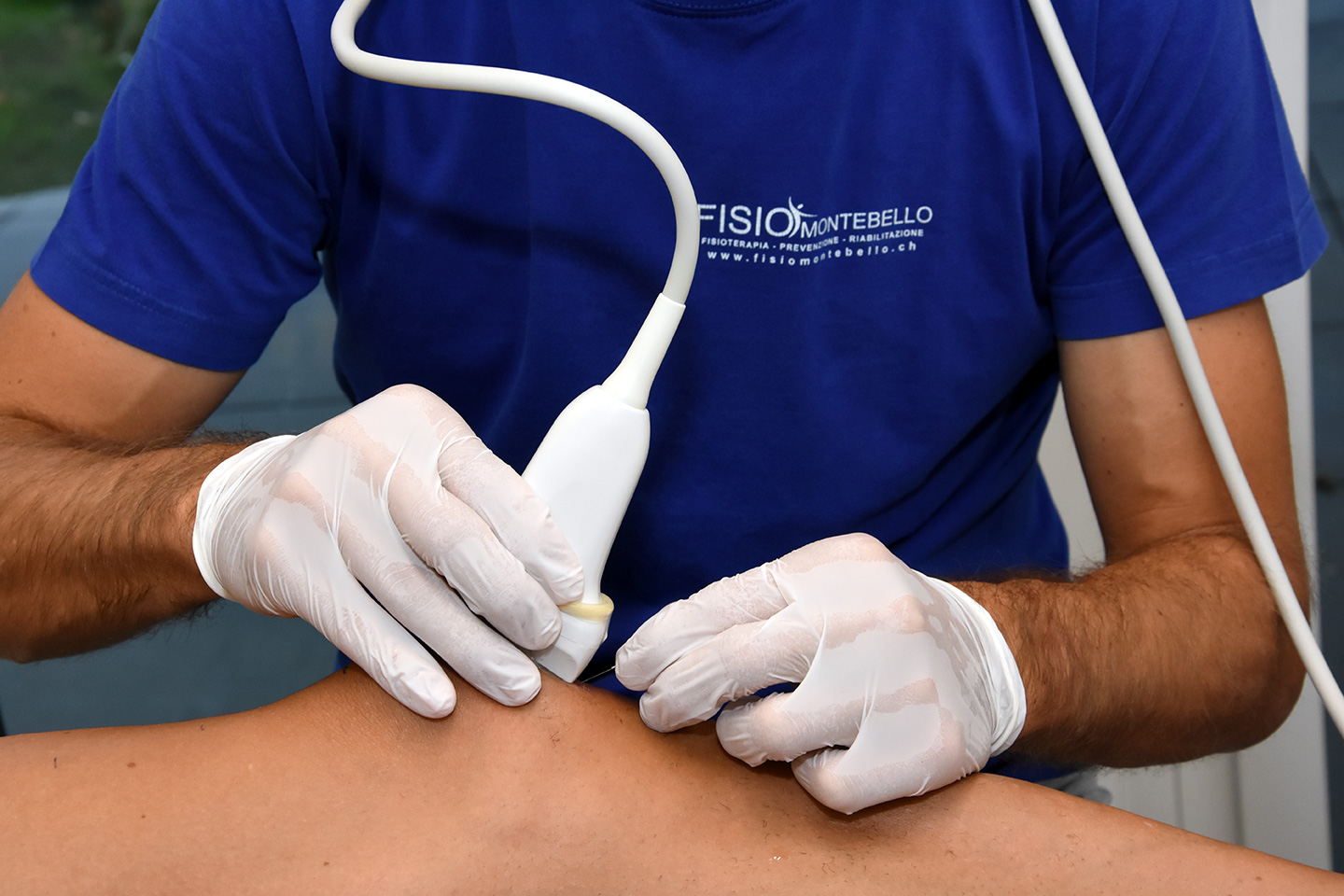
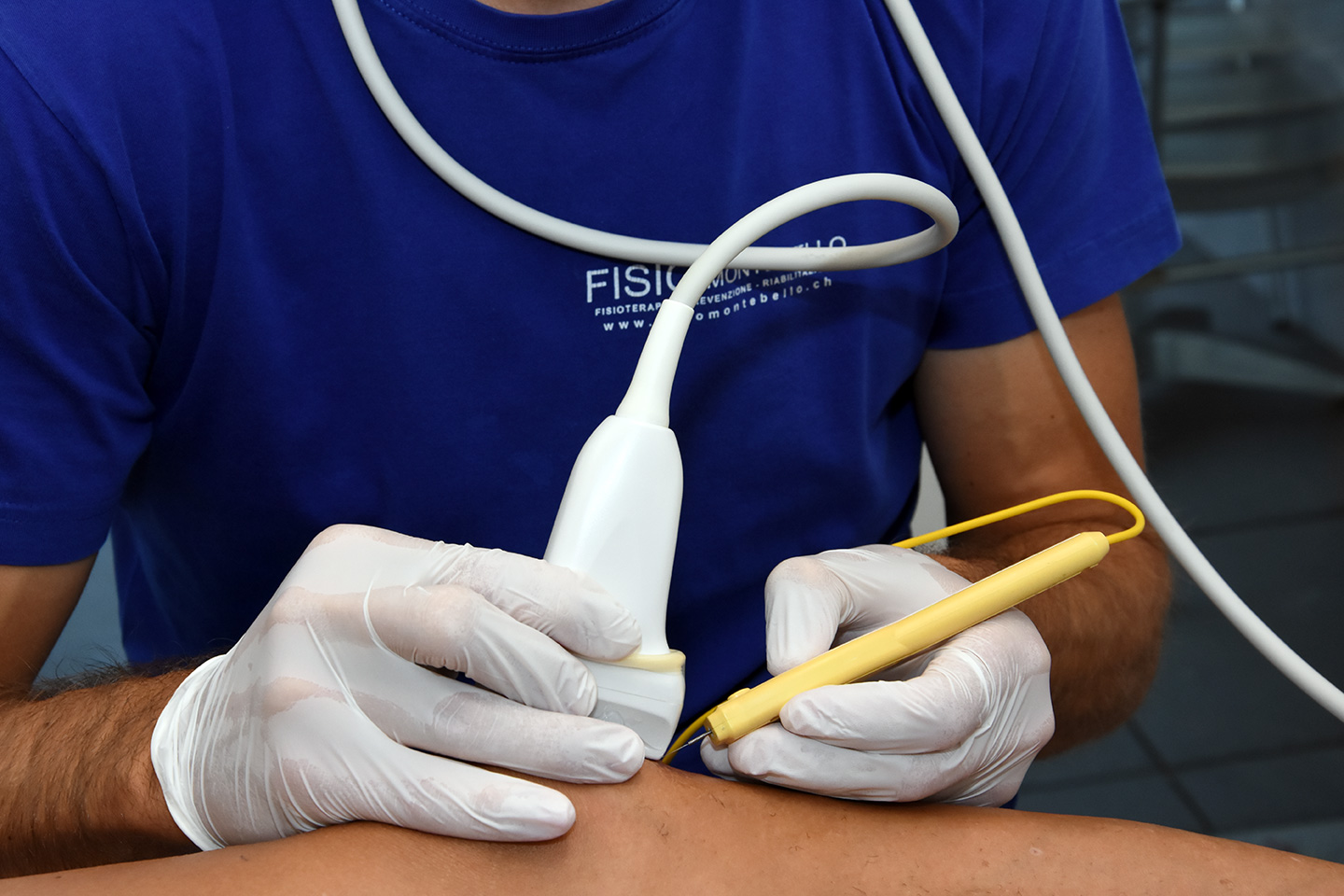
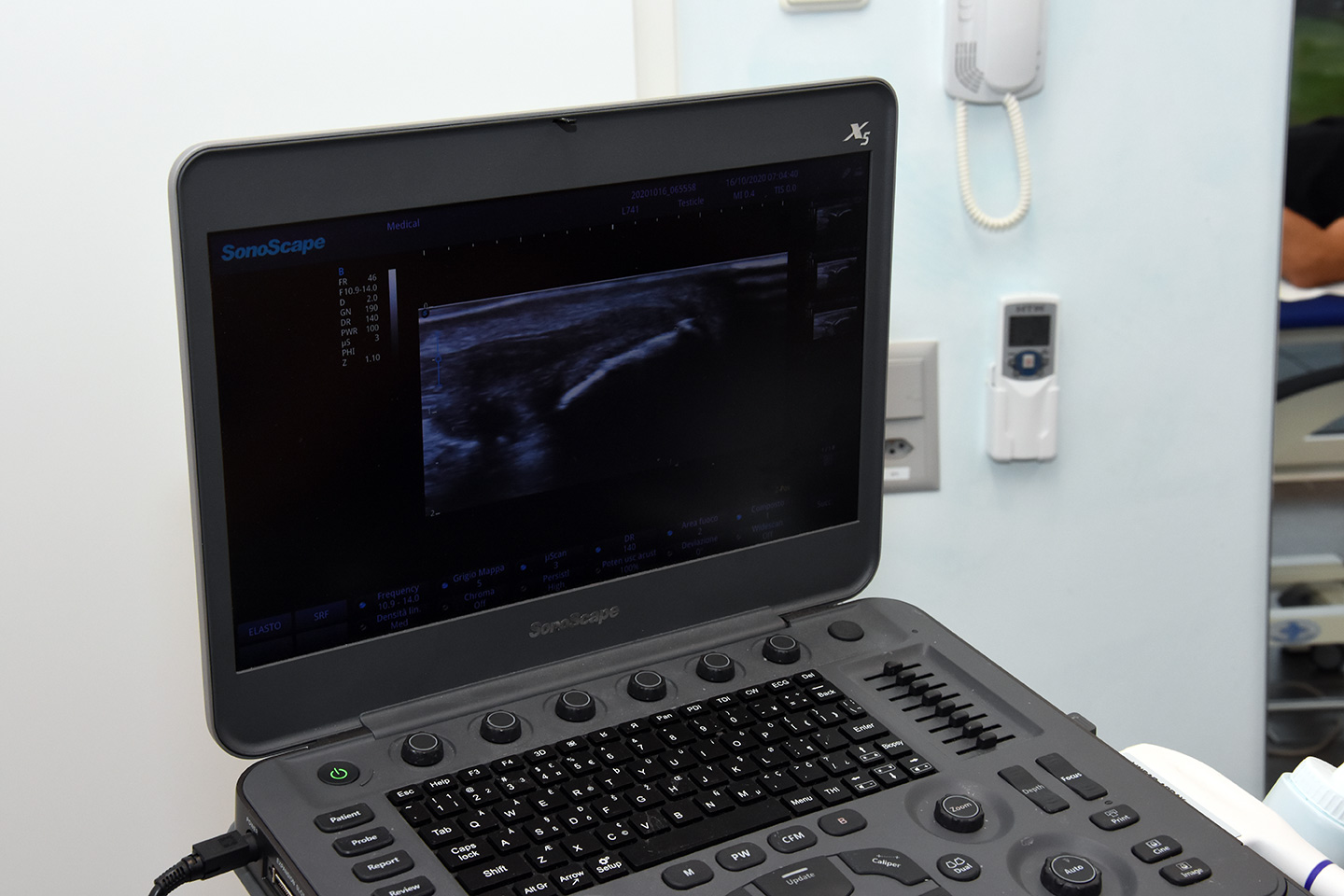
The EPM technique is indicated for:
- Chronic tendinopathies (patellar tendon, Achille’s tendon, pubalgia, lateral/medial epicondylitis, rotator cuff, supraspinatus tendon...)
- Bursitis (retrocalcaneal, deltoid bursitis, Achilles bursitis...)
- Acute and chronic muscle injuries
- Peripheral nerve entrapment syndromes
- Joint impingements
- Tenosynovitis (De Quervain's syndrome, tenosynovitis of tibialis posterior...)
- Tibial Periostitis
- Plantar fasciitis
- Acute and chronic muscle rupture (fibrosis)
- Myofascial trigger points
- Ligament sprain (medial collateral ligament of the knee, talofibular anterior ligament of the ankle…)
- Knee’s flexum (posterior joint capsule)
- Carpal and tarsal tunnel syndrome
- Anterolateral and posterior ankle impingement
- Adherent and painful scars
The advantages of the technique are:
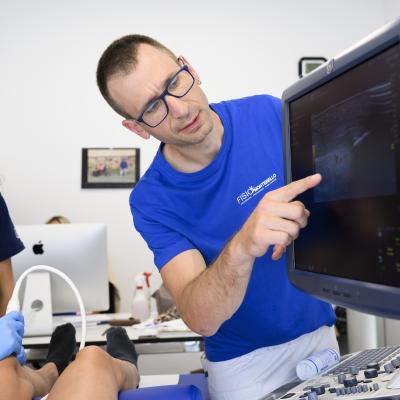
- It is a precise and local treatment that, with the help of an ultrasound, is performed directly on the altered and/or degenerated tissue. The precision of this technique is also ensured through the use of Power Doppler and elastography.
- When the rapier of connective tissue of a tendon or muscle is difficult, the EPM technique initiates a new process of collagen fiber proliferation, which in turn allows the repair process to resume in a physiological manner.
- The structural changes and mechano-biological behavior of soft tissue are immediate and in real time.
- The efficiency of EPM is high (about 70%) compared with both conventional physiotherapy (ultrasound, laser, Cyriax technique, diathermy therapy, shock waves, etc.) and other medical treatments (infiltrations or sometimes even surgery) in cases of neuro-musculoskeletal problems.
- The frequency of relapse is low.
In more chronic cases, electrolysis can also be combined with other invasive physiotherapeutic techniques:
- Neuromodulation (NMP_e)
- Microcurrents
- Bioregulation
- Intramuscular modulation (IMS)
- High-voltage currents
Contraindications:
- Belonephobia
- Acute systemic infections with or without fever
- Written permission for the invasive treatment is not granted by the patient
- All cases of acute emergency
- Osteosynthesis, prostheses, and implants (local contraindication)
- Pace Makers
- Heart disease where electric field charges could alter heart rhythm
- Skin problems (local contraindication)
- Thrombophlebitis
- Tumors
- Sensitivity disorders (relative contraindication)
- Lymph edema or situation of removal of lymph nodes (local contraindication)
- High risk of infection (relative contraindication)
- Metabolic alterations (relative contraindication)
- Fibromyalgia (relative contraindication)
- Pregnancy (absolute contraindication in the first trimester and in the subsequent months relative to areas that could affect the fetus)
- Children (parental permission required)
- Contagious diseases (relative contraindication)
- Allergies to the material used (relative contraindication, special measures required)
- Epilepsy (relative contraindication)
- Mucous membranes, eyes, genitals, nipples, and endocrine glands
Although it is a relatively new technique, there are already several studies showing its positive effect:
- Galvanic current activates the NLRP3 inflammasome to promote Type I collagen production in tendon
- A Molecular Mechanisms of Regeneration in Chronic Tendinopathy Using Ultrasound-Guided Intratissue Percutaneous Electrolysis (EPI®)
- Ultrasound-guided percutaneous needle electrolysis in chronic lateral epicondylitis: short-term and long-term results
- Ultrasound-Guided Percutaneous Needle Electrolysis and Rehab and Reconditioning Program for Rectus Femoris Muscle Injuries: A Cohort Study with Professional Soccer Players and a 20-Week Follow-Up
- Randomized controlled trial comparing the effectiveness of the ultrasound-guided galvanic electrolysis technique (USGET) versus conventional electro-physiotherapeutic treatment on patellar tendinopathy
- Intratissue Percutaneous Electrolysis vs Corticosteroid Infiltration for the Treatment of Plantar Fasciosis
- Treatment of proximal hamstring tendinopathy-related sciatic nerve entrapment: presentation of an ultrasound-guided "Intratissue Percutaneous Electrolysis" application
- The Effectiveness of Minimally Invasive Techniques in the Treatment of Patellar Tendinopathy: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
- Ultrasound-Guided Percutaneous Needle Electrolysis in Dancers with Chronic Soleus Injury: A Randomized Clinical Trial
- Percutaneous Needle Electrolysis Accelerates Functional Muscle Regeneration in Mice
Studies conducted in Spain have shown that damaged tissue can potentially be treated through the EPM procedure rather than surgery. This implies that the affected tendon or area is able to heal without the need for invasive surgery.