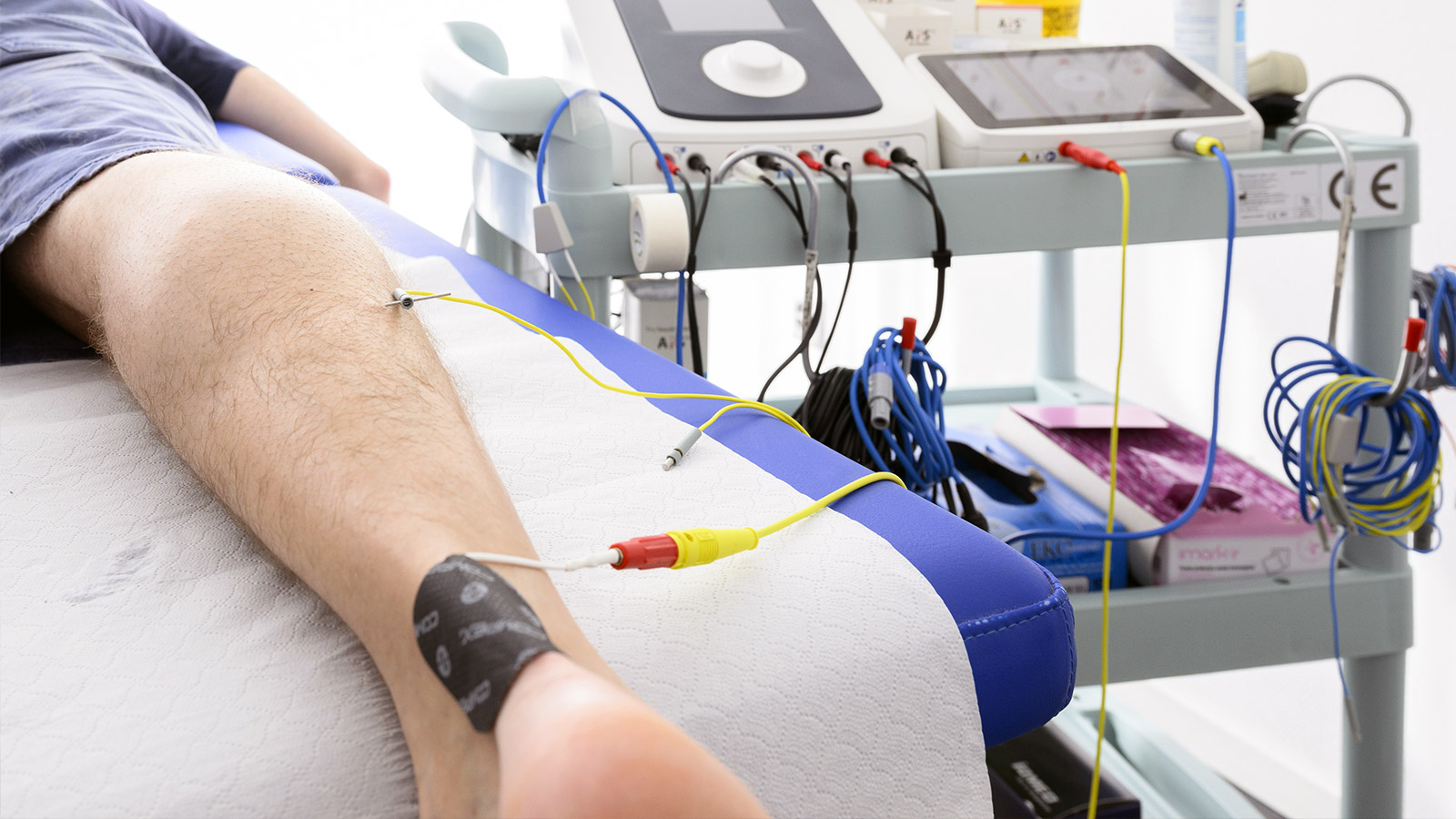
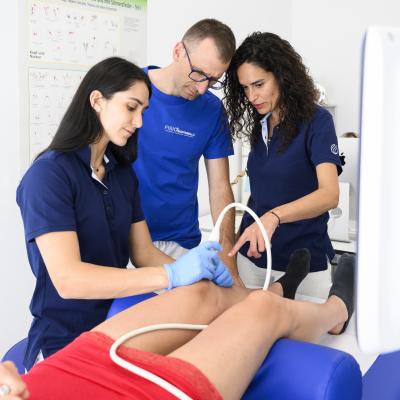
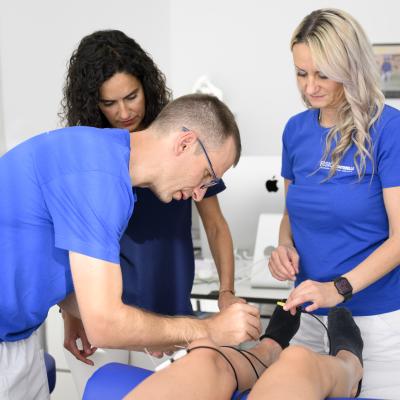
Percutaneous ultrasound-guided neuromodulation (NMP_e) or peripheral neuromodulation is a technique that consists of the ultrasound-guided introduction near a peripheral nerve of acupuncture needles, connected to a low- or medium-frequency alternating electric current device. Stimulation of the peripheral nerve at its motor point leads to a sensory, motoric or autonomous response.
This technique is often combined with percutaneous electrolysis (EPM), which instead directly treats the injured tissue. The combination of these two techniques is very effective, as both the structure and its function are treated.
It is applied to treat different neural structures in relation to a previous assessment of the patient's symptomatology and dysfunction in order to promote changes in the peripheral and central nervous system by modulating the abnormal behavior of the neuronal pathway caused by the disease process or the dysfunction.
The introduction of this technique into clinical practice makes it possible to accelerate recovery time. It can also be adopted as a preventive approach to dysfunction once the lesion has been treated. It is a painless, safe technique that is well tolerated by patients.
For maximum accuracy and safety, it is essential that the technique is applied using a next-generation ultrasound scanner (sonographer) that is suitable for this kind of approaches.
The main goals of neuromodulation are:
- The treatment of acute and chronic pain of musculoskeletal origin (spine and limb pain, postoperative pain...)
- The treatment of neuropathic pain
- The restoration of peripheral and central nervous system function in aspects related to sensory or motor dysfunction
- The improvement of neuromuscular function, muscle recruitment pattern and motor control
- The improvement of proprioception
Indications:
- Herniated disc, cervicobrachialgia, sciatica
- Headaches, cranial neuralgia (Arnold neuralgia, trigeminal neuralgia...)
- Pain of the temporomandibular joint (TMJ)
- Neuropathic pain (pain generated by neural damages)
- Nerve entrapment syndrome (piriformis, femoral quadratus-gluteus maximus, tarsal tunnel, Baxter's syndrome...)
- Musculoskeletal pain
- Reduced neuromuscular activation and control, proprioception deficit
- Loss of sensation
- Joint instability
- Muscle ruptures
- Prevention of muscle injuries
Contraindications:
- Belonephobia
- Acute systemic infections with or without fever
- No clear agreement by the patient for the treatment with IP
- All cases of acute emergency
- Osteosynthesis, prostheses, and implants (local contraindication)
- Pace Maker
- Heart disease where electric field changes could alter heart rhythm
- Skin problems (local contraindication)
- Thrombophlebitis
- Tumors
- Sensitivity disorders (relative contraindication)
- Lymph edema or situation of removal of lymph nodes (local contraindication)
- High risk of infection (relative contraindication)
- Metabolic alterations (relative contraindication)
- Anticoagulation therapy and coagulation problems (INR value must be greater than 1.5 in order to be treated)
- Fibromyalgia (relative contraindication)
- Pregnancy (absolute contraindication in the first trimester and in the subsequent months relative to areas that could affect the fetus)
- Children (parental permission required)
- Contagious diseases (relative contraindication)
- Allergies to the material used (relative contraindication, special measures required)
- Epilepsy (relative contraindication)
- Mucous membranes, eyes, genitals, nipples, and endocrine glands
As the technique is very new (2017), there are still few studies about it, but considering the huge positive clinical effect they will soon be published.
- A Review of Peripheral Nerve Stimulation Techniques Targeting the Medial Branches of the Lumbar Dorsal Rami in the Treatment of Chronic Low Back Pain